What Is Age-Related Macular Degeneration (AMD)?
Reviewed by: HU Medical Review Board | December 2018 | Last updated: September 2023
Among older adults in industrialized nations, age-related macular degeneration (AMD) is the primary cause of visual impairment and blindness.1 It affects the macula, an oval-shaped area near the center of the retina that is important for central vision or seeing straight ahead of us.
In AMD, sizeable yellow deposits called drusen may develop under the retina. While a few small drusen may be a normal byproduct of aging, larger drusen can be a sign of AMD. If the macula is damaged, it can cause a blurry or dark spot in the middle of your field of vision. The progression of AMD can vary, and treatment is different depending on the stage of disease.
Stages of AMD
There are three stages of AMD, and these are generally based on the size and number of drusen present. AMD might only be present in one eye or found in both, and the severity can vary in each eye. The three stages include2:
Early AMD
- Several small or medium-sized drusen are present and are approximately the width of a human hair
- Patient might be asymptomatic otherwise, with no reported vision impairment
Intermediate AMD
- Numerous medium-sized drusen or at least one large drusen is present
- There may also be pigmentary changes in the retina
- Vision loss might be reported, however most patients are still asymptomatic
Advanced AMD
- Along with drusen, the macula is damaged, causing vision loss or impairment
Types of AMD
- Dry AMD (Geographic atrophy): Slow breakdown of cells in the macula that send images to the brain, as well as a breakdown of the supporting macular tissue, causing loss of vision
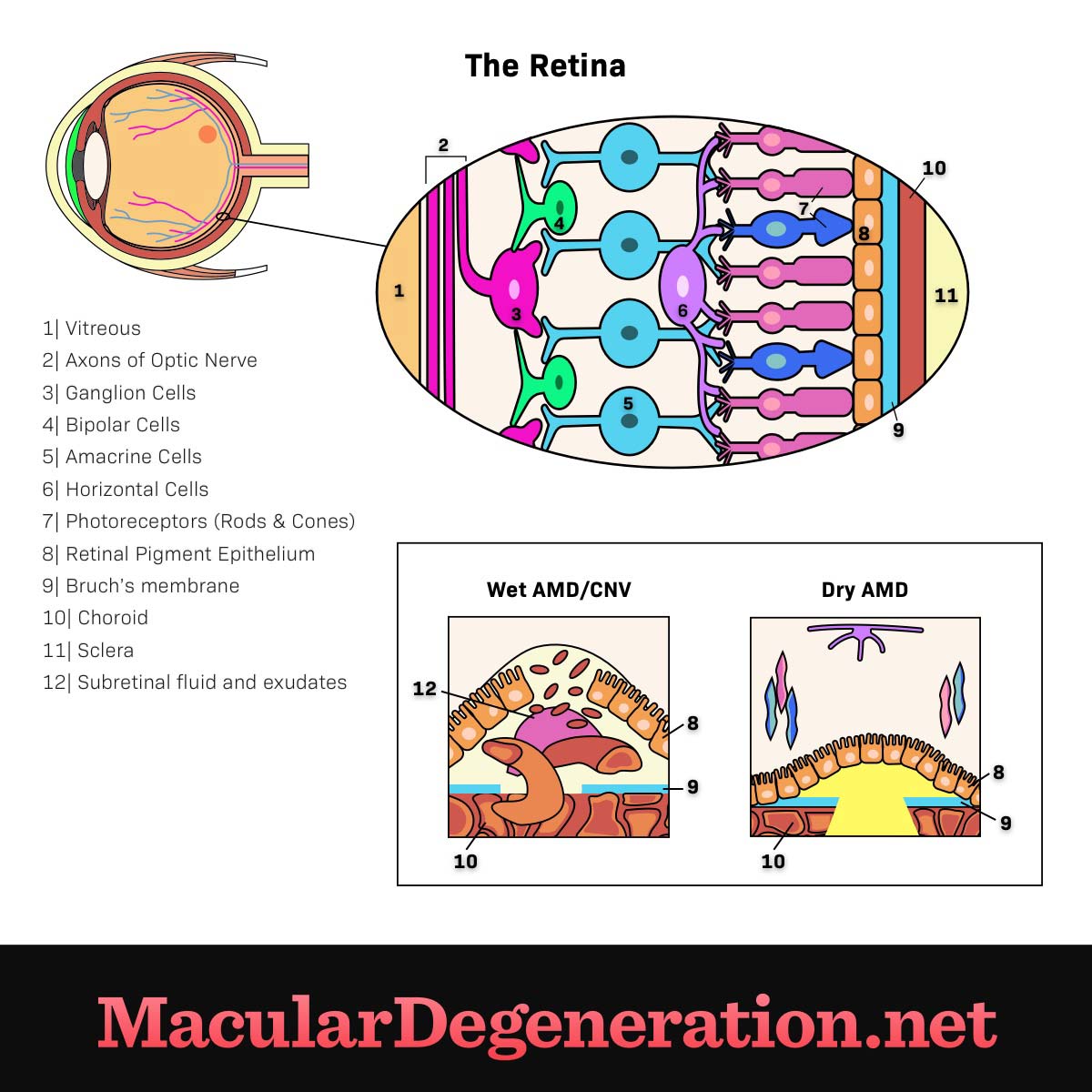
- Wet AMD (Neovascular AMD): abnormal blood vessels are found growing under the retina, possibly leaking or bleeding and causing damage to the macula; the damage can occur suddenly and be quite severe
Figure 1. Wet vs. dry AMD
It is possible to have both types of AMD in the same eye. While approximately 90 percent of AMD patients have dry AMD, wet AMD is more often associated with central vision loss.1 Not everyone with early AMD will go on to develop intermediate or late AMD. Once early AMD is diagnosed, there are lifestyle changes and vitamin supplements that may help reduce the risk of AMD progression.
AMD pathophysiology
Age-related macular degeneration (AMD) is a disease of the macula, the center of the retina. It impacts central vision and is most prevalent in those over the age of 50.3 It appears that AMD arises from damage to the retinal pigment epithelium (RPE) and Bruch’s membrane (BM).3,4 When the RPE and BM start breaking down, waste products that would normally be recycled begin to accumulate underneath the retina, forming into drusen. Drusen are markers of dry AMD that may appear even in the early stages of the disease before any changes in your vision.
Early signs of AMD
Another early sign of AMD that your doctor can find with a dilated eye exam are pigmentary changes under the retina. When the RPE cells break down, the pigment is released, causing clumps of pigment to form.5 This won’t change your eye color and won’t be noticeable to the general individual, but your eye doctor will be able to see the clumps underneath the retina, and may also be able to see areas that are lacking pigment.
Neovascular AMD pathophysiology
In wet AMD, also called neovascular AMD, the growth of new, abnormal blood vessels under the retina occurs; hence the term “neovascular.”5 These blood vessels form because the eye is trying to get more oxygen and nutrients to an area damaged by dry AMD, similar to the healing response seen after a scrape or cut. These blood vessels usually arise from the choroid and break through weak areas in Bruch’s membrane to enter the retina. However, the walls of these new abnormal blood vessels tend to be weaker and prone to leaking or bleeding, which may result in rapid damage to the macula with associated vision loss. Whereas dry AMD typically has a slower progression, vision loss from wet AMD can be very sudden.
Diagnosis of AMD
Because AMD is asymptomatic, or causes no symptoms, in the early stages, it’s important to have regular eye exams by a professional – especially if you’re over the age of 50.6 An eye doctor can perform tests like a visual acuity test, dilated eye exam, or an Amsler grid. More invasive tests are sometimes done but are generally not the first-line in diagnosis.
Risk Factors for AMD
The main risk factor for AMD is age. Patients with AMD are usually age 50 or older, with the prevalence of AMD increasing with age.1,6 Advanced AMD is seen more often in Caucasian patients than in African-American or Latino/a patients.
Lifestyle factors
There are some lifestyle factors that can impact your risk of developing AMD, including:
- Smoking: Smoking doubles the risk of developing AMD1
- Nutrition and Exercise: Exercise regularly and eat a healthy balanced diet, especially green leafy vegetables and fish
- Blood Pressure and Cholesterol: Keep blood pressure and cholesterol levels under control
AMD is treatable, but an important factor is an early diagnosis. Prompt treatment can help you maintain vision and address any vision loss you might already have. Although there is no treatment yet for early AMD, being aware of any changes is key, and adopting healthy lifestyle habits might have positive effects on the course of your AMD.