Through the Looking Glass: Your Journeys With Macular Degeneration
You woke up one morning and noticed your vision looked blurry and all of a sudden a blind spot shows up out of nowhere! You make an appointment with your eye doctor and are soon after are diagnosed with macular degeneration. You immediately think of what your mother’s experience with it was - what did she have trouble with? Later that night as you’re taking your blood pressure medication you begin to map out the changes you need to make in your life to save your remaining vision.
Sound familiar?
800 respondents from our 2nd Annual Macular Degeneration In America survey told a very similar story.
Changes in your vision
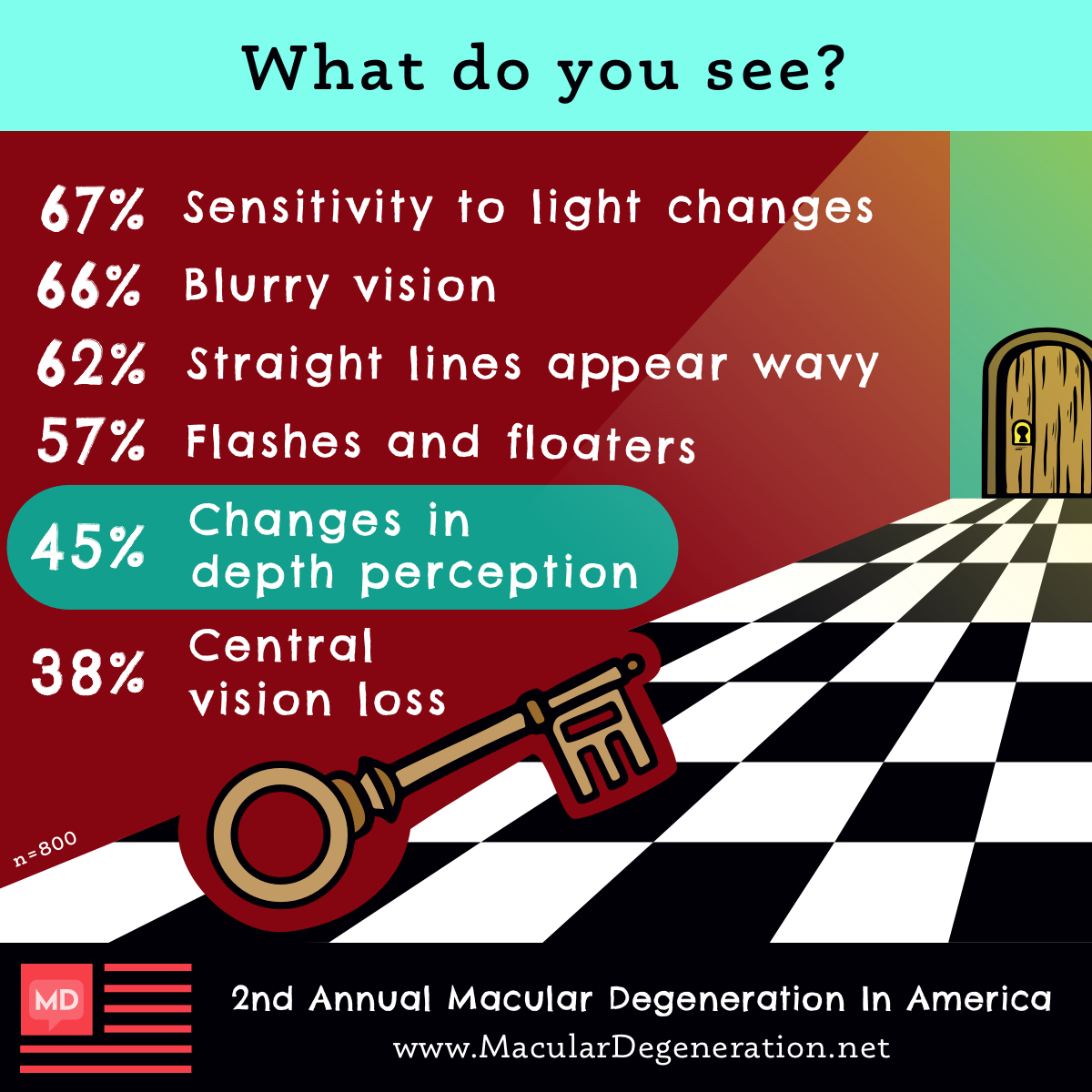
Some visual symptoms develop gradually over time, while others can feel like they hit - BAM! - out of nowhere. From blurriness and floaters to difficulty with recognizing faces, many of you have shared that macular degeneration can be both really frustrating and really frightening and makes quotidian tasks – cleaning, reading, driving, even just clipping your fingernails – extremely difficult if not impossible. Here are some of the most common macular degeneration symptoms experienced among the community:
A dry or wet macular degeneration diagnosis
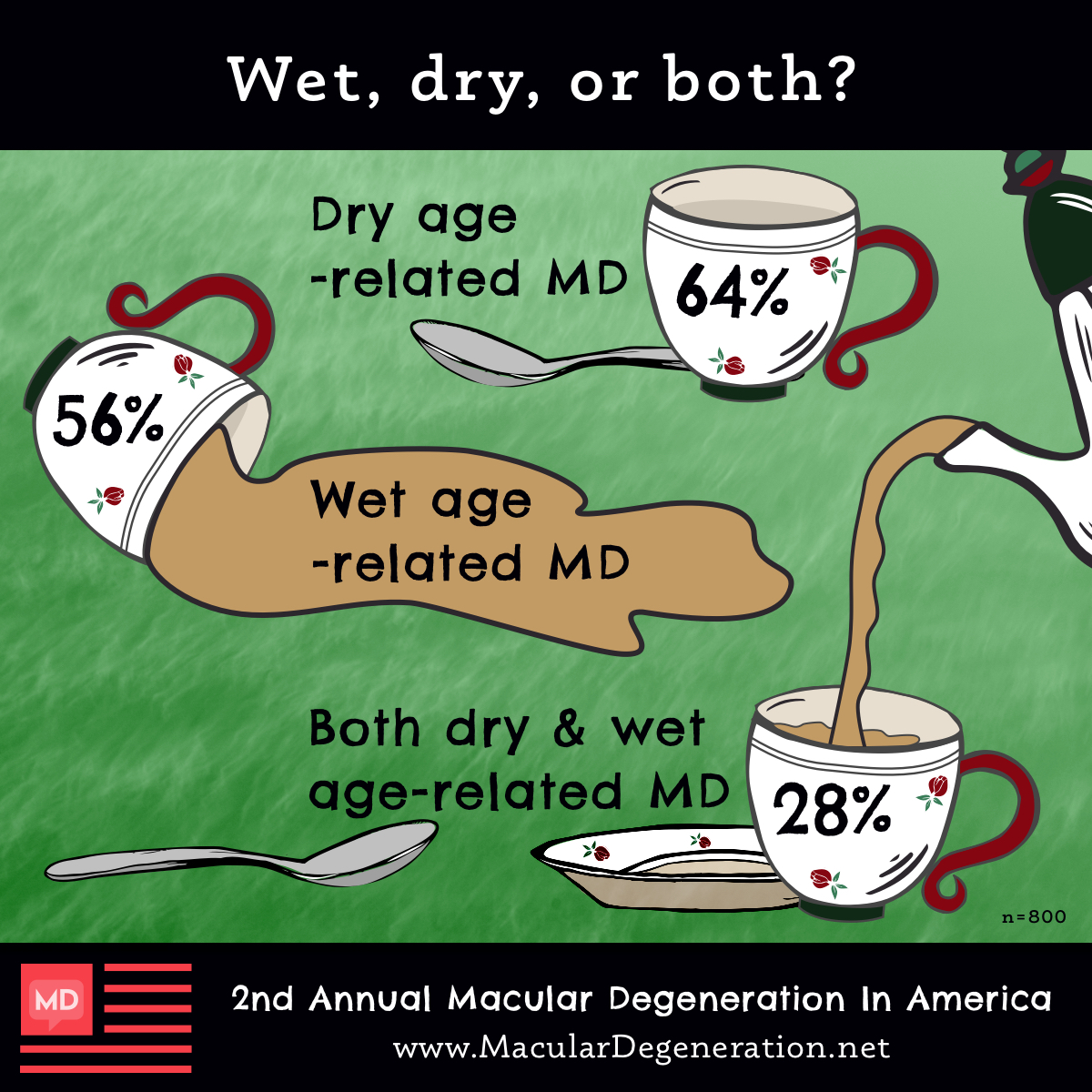
A macular degeneration diagnosis doesn’t always occur in the thick of vision loss symptoms. It can be diagnosed in the earliest of stages, also known as early dry AMD, or in the later and more advanced stages where it branches off into wet AMD or advanced dry AMD, also known as geographic atrophy. Where you were at your diagnosis might be different from where you are now. Many of you were around 65 years old when you began to notice symptoms of macular degeneration and were diagnosed around 67 years old. But, were you diagnosed with wet or dry macular degeneration? There’s a big difference!
Macular degeneration is a family affair
Although there are various risk factors that can increase your risk for developing macular degeneration, studies have shown that there is a hereditary component to this condition. We asked you in our survey if any of your family members have also suffered from macular degeneration, and we were surprised to learn that more than ¼ of you cited that your mother also has or had macular degeneration.
Managing more than vision loss
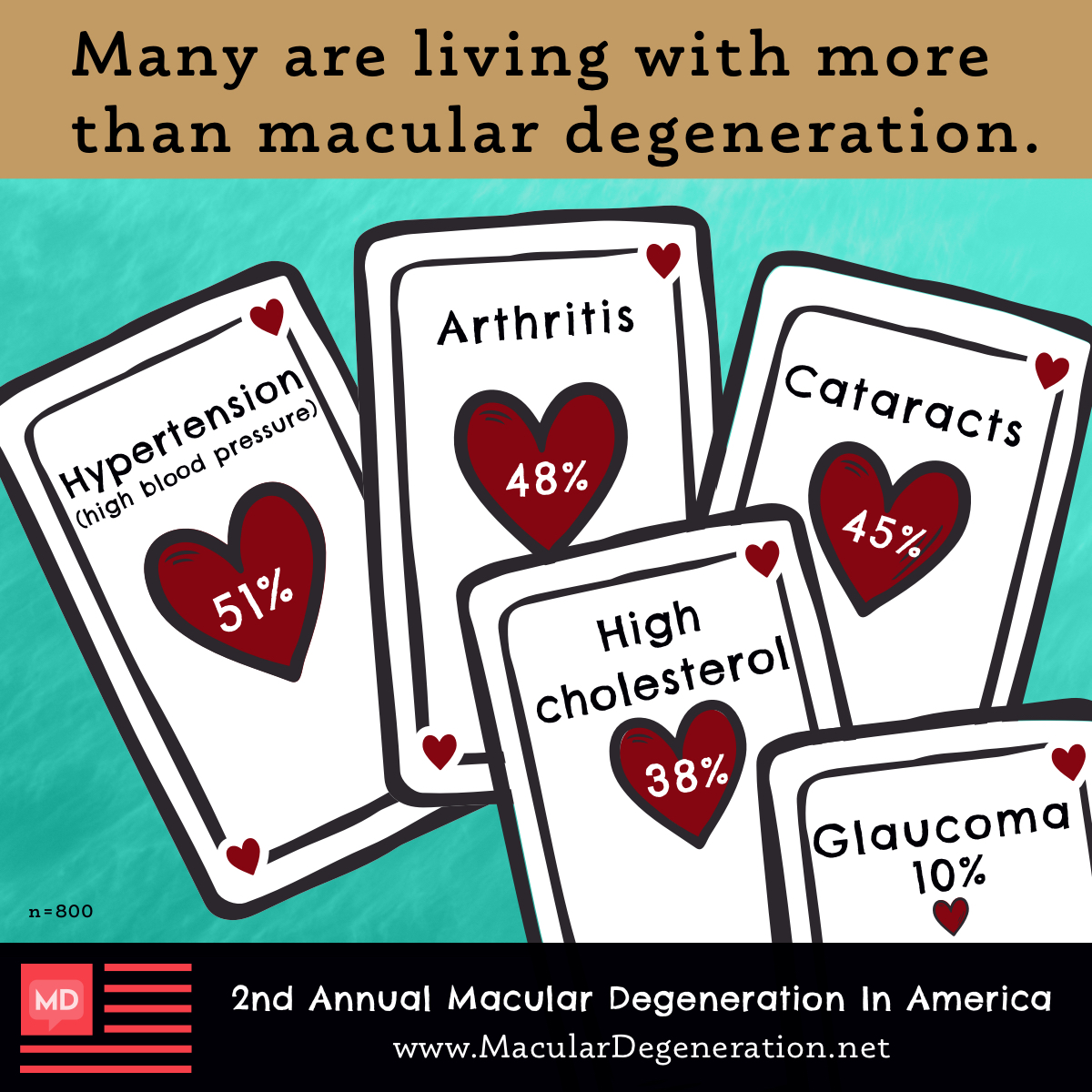
Macular degeneration is enough of a handful on its own, but our survey results revealed that many in the community have a lot more on their plate. In particular, many of you shared that you’re also juggling hypertension, arthritis, and osteoporosis as well as other eye conditions like cataracts and glaucoma.
Vision loss changes everyday life
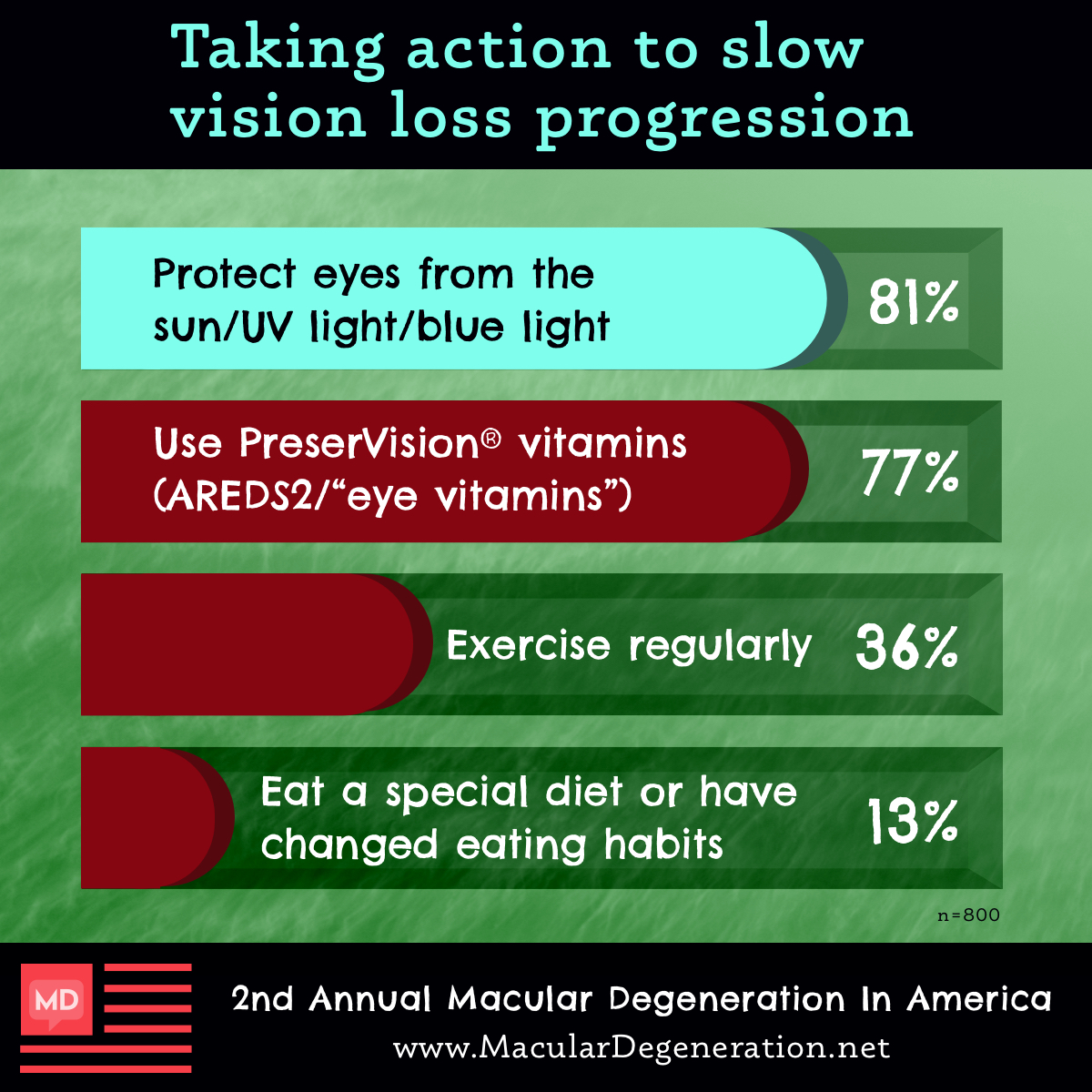
As you begin to think about what lifestyle changes you’re going to have to make, outside of finding other modes of transportation or magnifying the screen to read an e-book, your goal becomes preserving your vision and slowing progression. In this case, it’s about taking those eye vitamins and supplements, such as the AREDS2 formula, going for a 15-minute walk each day or some other form of physical activity, or even making yourself dinner and modifying it to fit the Mediterranean diet. Added up, these small changes can make a big difference in everyday life, and many of you have made them in an effort to save your sight.
The Macular Degeneration in America 2020 survey was conducted online from December 2019 through March of 2020. 800 people completed the survey, all had to be diagnosed with some form of macular degeneration to qualify.


Join the conversation